Thank you to all participants
DREAMBIG could not exist without the generosity and the implication of all participants.
RECENT FINDINGS
Negative Emotionality
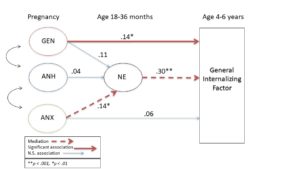
Figure 1. Early NE as a mechanism underlying the relationship between clusters of maternal prenatal psychopathology and childhood internalizing problems
Not everyone is susceptible to the effects of prenatal stress. Part of the initiative of the Maternal Adversity Vulnerability And Neurodevelopment (MAVAN) project is to further understand child characteristics that may make some children more susceptible to prenatal maternal psychological stress. The MAVAN project was started to explain the effect of early life stressors on child development and it consists of a community cohort of over 500 mother-child dyads from Montreal, Quebec and Hamilton, Ontario. Currently, work by Cathryn Gordon Green and colleagues using data from the MAVAN project directly evaluates the role of prenatal maternal stress on Negative Emotionality (NE), a child temperamental trait that develops early in infancy. NE, which reflects sadness, fear and emotional over-reactivity, is linked to maternal mood during pregnancy and the development of later psychopathology in childhood and adolescence. In a three-part study, we aim to uncover the developmental trajectory of internalizing psychopathology in preschool age children by examining the predictive role of prenatal maternal psychopathology and early child NE.
Important findings from the first study (Gordon Green et al., 2017) demonstrate a link between prenatal maternal psychopathology and the development of NE between 3 and 36 months that is moderated by child genetic risk. Only children with certain genetic variants who were exposed to prenatal maternal psychopathology were subsequently rated higher in NE by their mothers. The second study (Gordon Green et al., paper in prep) aims to examine the role NE in a larger model examining the impact on preschool internalizing problems. Findings reveal NE mediates the relationship of prenatal maternal psychopathology and preschool internalizing symptoms and identifies NE as one potential mechanism through which maternal prenatal psychopathology influences later childhood internalizing psychopathology. The last study will be a continued investigation of how the relationships between maternal psychopathology, NE, and child internalizing problems might differ based on child genetic vulnerability.
The findings from these studies have important implications for prevention and intervention programs. Treatments targeting prenatal maternal psychopathology have helped to reduce maternal symptoms, however, it is unclear if they also act to improve child outcome. We identify early child characteristics that can serve as additional targets for intervention for women with prenatal psychopathology to facilitate more optimal outcomes for their children.
Infant Sleep
Sleep plays a fundamental role in child development, and a growing body of evidence suggests that lack of sleep in infants is associated with both physical and mental health problems. Sleeping through the night somewhere between six to twelve months of age is generally considered the “gold standard” in Western nations. However, the idea of night awakenings as being problematic in early development is not unanimous, leading to conflicting advice from professionals.
Pennestri et al.(2018) used data from the Maternal Adversity, Vulnerability, and Neurodevelopment (MAVAN) longitudinal birth cohort, to investigate whether 6-12 month-old infants uninterrupted sleep through the night, in 6 or 8 hour sleep blocks, have associations with mental and psychomotor development, maternal mood, and breastfeeding. They reported that 27.9% to 57.0% of 6- and 12-month-old infants did not sleep through the night. Moreover, a higher percentage of girls than boys slept through the night at some time points. Notably, no associations were found with infant sleep patterns and variations in mental or psychomotor development of the infant or maternal mood. However, the results revealed a strong relationship between breastfeeding and not sleeping through the night.
This study demonstrates that infants sleep cycle does not seem to have an effect on their mental or psychomotor development, which has important implications for parenting. New parents appear to be greatly surprised about the degree of sleep disturbance and exhaustion that they experience. Parents can benefit from being informed about the normal development of the sleep-wake cycle.
Dysregulation
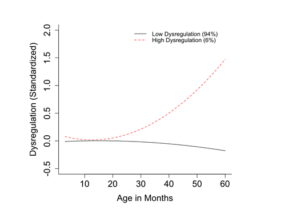
Figure 1. Trajectory of Dysregulation from 3 to 60 Months (N = 582)
Childhood dysregulation is a triad of impairment in the child’s ability to self-regulate their emotions, thoughts, and behaviours, and has been associated with comorbid mental health disorders (i.e. the simultaneous presence of two or more disorders) throughout childhood and beyond. We investigated the origins of childhood dysregulation by examining risk factors that could be targeted for prevention and early intervention. These factors included maternal depressive symptoms pre- and post-pregnancy, fetal exposure to psychotropic medication, infant and early childhood temperament, variation in child genotypes that had previously been associated with psychiatric disorders (e.g. serotonin and dopamine related genes), biological sex, and socioeconomic factors such as family income and education background. Our assessments included yearly mother reports of their mental health and of their child’s mental health and ability to regulate (i.e. dysregulation), laboratory observations, psychiatric interviews, and genotyping.
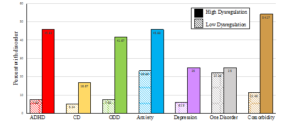
We found that maternal pre- and postnatal depression and child genotype interacted to predict childhood dysregulation from 3 months to 6 years of age, and that prenatal exposure to psychotropic medication did not put children at a greater risk for dysregulation. We also found that there are two developmental trajectories (i.e. two groups) for dysregulation from 3 months to 6 years of age. As see in Figure 1, 94% of the children were in the “low dysregulation group” and represented those children did not have dysregulation problems, whereas the other 6% of the children were in the “high dysregulation group” and represented those children who did have dysregulation problems. We then found that children who were in the high dysregulation group were two to six times more likely of having a psychiatric disorder at 6 years of age, such as ADHD, anxiety, depression, oppositional defiant disorder, and conduct disorder, and nearly five times more likely of having comorbid psychiatric disorders (i.e. 2 or more disorders at the same time), as seen in Figure 2.
Figure 2. Distribution of Disorders in Low vs. High Dysregulation Groups
Our aim is to provide researchers, clinicians and policy makers with target risk factors in the development of dysregulation and associated childhood psychiatric disorders, in order to promote early prevention and intervention that benefits the mental health and development of women and their children.
NEXT PROTOCOL
Evaluation at 13 years – Child and Adolescent Psychiatric Assessment (CAPA)
When children are between the ages of 9 to 16 years old, over 30% will develop at least one psychiatric disorder, such as disruptive behavior disorders (e.g. attention deficit hyperactivity disorders (ADHD), oppositional defiant disorder (ODD), conduct disorder (CD), mood disorders (e.g. major depression, dysthymia, mania and hypomania), anxiety disorders (e.g. generalized anxiety disorder (GAD), specific phobia, social phobia, post-traumatic stress disorder (PTSD), selective mutism, eating disorders, sleep disorders, elimination disorders (i.e. enuresis and encopresis), substance use disorders, and schizophrenia. At this age, puberty and entry into high school are among the known stressors that can lead to mental health problems. Further, girls are twice as likely to experience a depressive episode than boys, a gap that persists well into adulthood.
Much research is needed on childhood causes and protective factors of psychiatric disorders if prevention programs are to be effective, and studies that follow the same children over time are one of the best sources to provide this kind of information. Identification and treatment of mental illness can help parents and children overcome the trajectories of these disorders, taking advantage of the plasticity of the young brain. Identification requires developmentally appropriate measures of impairment in three different settings: home, school, and other settings in the community, as well as assessment of how symptoms affect the child’s relationships with parents, siblings, friends, and other adults such as teachers.
In the MAVAN study, we identify childhood psychiatric disorders with the Child and Adolescent Psychiatric Assessment (CAPA), a psychiatric interview that assesses DSM-IV and ICD-10 psychiatric symptoms and disorders in children ages 9-17 years. The CAPA was developed by Adrian Angold MRCPsych and Jane Costello, both child psychiatrists and epidemiologists at the Center for Developmental Epidemiology in the Department of Psychiatry and Behavioral Sciences at Duke University Medical Center. The CAPA assessments take place during the child’s first year of high school, when they are 13 years old.
Want to know more about this research?
Maternal Adversity, Vulnerability and Neurodevelopment (MAVAN) - Child Mental Health Resilience and Susceptibility in the COVID Pandemic
COVID-19 and our research: The global COVID-19 pandemic has resulted in widespread changes to how we live our lives. The pandemic has also led to a high number of illnesses and deaths both in Canada and worldwide. The result has been a toll on the physical and mental health of Canadian adults and children. Our research has always aimed to understand both personal and environmental factors that can influence the development of children and adolescents; it’s therefore important for us to understand how this pandemic has affected the lives of families such as, those who have participated in the Maternal Adversity, Vulnerability and Neurodevelopment (MAVAN) study since birth.
What we are proposing: In this phase of the study we are looking at the effect of a major stressor (COVID-19) on mothers and their children and how this stress can interact with earlier life experiences to influence current and future child functioning.
The objective of this phase of the research project is to see whether exposure to the COVID-19 pandemic affects child functioning differently, depending on their genes and foetal development (a concept known as “prenatal programming)” and other developmental factors.
What we are proposing continued: Several factors can influence how adults and children are affected by major stressors in their lives: previous experiences, moods, and behaviors, levels of social support, coping strategies, levels of resilience, gender, and genes. Thanks to the dedication of the MAVAN families, we have been able to collect a wealth of information on these and other important factors, which may be used to determine just how resilient children can be when faced with a very challenging and stressful global crisis.
Participation and assessments: For these purposes, we will ask participants (both mothers and children) to take part in an online interview and complete a series of online questionnaires about their experiences during the COVID-19 pandemic. It will take about 90 minutes for the mother and 60 for the child to complete the questionnaires using a secure online survey program called REDCap. We will also ask the children’s teachers to complete a few online questionnaires about the children’s functioning at school.
Please click here for a table and description of the questionnaires and interviews that will be administered during this research project.
Benefits for participating: Your participation, and that of your child, will help us determine if past experiences, feelings, behaviors you and your child have experienced can serve to protect against the stress associated with the COVID-19 pandemic. There are no anticipated risks of participating in this research project, and you will be able to withdraw from this project at any time.
How to participate: We will soon be launching this important phase of the MAVAN study. All MAVAN families who remain active participants will receive an email explaining the study in more detail and asking whether they would like to assist us in understanding how mothers’ and children’s past experiences, moods, behaviors explain how the COVID-19 pandemic might influence current and future child functioning.
As always, we thank all the MAVAN families for their past and current interest in our study.
Want to know more about this research?
RECENT PUBLICATIONS
DREAM BIG PRESENTATION
1. Wazana A (2018). Dream-Big: Complex and novel approaches to studying developmental psychopathology
a. Wazana A, Jolicoeur-Martineau A, Szekely E, Greenwood C
The Latent Environmental and Genetic InTeraction model
(LEGIT): The next step in GxE interaction testing
b. Szekely E, Neumann A, Sallis H, Pearson R, Tiemeier H, Evans J, Wazana A
Does it matter for the offspring what stresses the mother during pregnancy?
A longitudinal, multi-cohort study of antenatal maternal stress and early
life offspring psychopathology
c. King L, O’Donnell K, Jolicoeur-Martineau A, Szekely E, Wazana A
Resilience in the context of Cumulative Early Life Adversity
d. Marshall C, Gordon Green C, King L, Szekely E, Wazana A
Environmental and child characteristics as moderators of the relationship
between prenatal depression and early child internalizing problems
Book of Abstracts – Symposium
2018 World Association for Infant Mental Health
Rome, Italy (May 2018)
2. Wazana A (chair) Lahey B (discussant). (2017). DREAM BIG – An international multi-site collaboration modelling the complex prediction of psychopathology.
a. Wazana A, Jolicoeur-Martineau A, Szekely E, Greenwood C, Sassi R, Kennedy J, Meaney M
GxE modelling with weighted genetic score and weighted environmental score
Book of Abstracts – Symposium
International Society for Research in Child and Adolescent Psychopathology Biennial Scientific Meeting
Amsterdam, Holland (July 2017)
MAVAN PUBLICATIONS
Jolicoeur-Martineau A, Wazana A, Székely E, Kennedy JL, Meaney MJ, Greenwood C.M.T. and the MAVAN team (2019) Alternating optimization for G×E modelling with weighted genetic and environmental scores: Examples from the MAVAN study. Psychological Methods, 24(2), 196-216.
Wazana, A. (2017). Les jeux ne sont pas faits à la naissance! Le furet. 87.
Graffi J, Moss E, Jolicoeur-Martineau A, Tsabari G, Lecompte V, Pascuzzo K, Babineau V, Gordon-Green C, Mileva V, Minde K, Sassi R, St-André M, Carrey N, Steiner N, Kennedy JL, Gaudreau H, Levitan R, Meaney M and Wazana A for the MAVAN project. (2015). The Effects of Small Birth Weight for Gestational Age and Polymorphisms of the Dopamine D4 Receptor Gene on Attachment Styles of Preschool Children. McGill Student Undergraduate Research Journal, 10, 30-36.